Have you ever thought about how unbalanced our understanding of a speech sound disorder is compared to a language disorder? On the language side we are really comfortable with some very technical words like morphology, syntax, and pragmatic use. But what has speech sound disorders research given us? We have articulation and phonology. Going past that, maybe we can head into completely different camps that affect speech like VPI, hearing, and stuttering. But, our treatment of typical unintelligibility is kind of limited.
Speech vs. Language
| Speech | Language |
|---|---|
| Articulation | Receptive |
| Phonology | Expressive |
| ? | Syntax |
| ? | Pragmatics |
| ? | Morphology |
| ? | Semantics |
Shouldn’t we have a better description of the many different ways a child is unintelligible? And if we can get there, shouldn’t there be different ways to treat those areas? I mean, you wouldn’t do semantic therapy with a child who has grammar goals. And you wouldn’t focus on pragmatic language for a child when the concern is that they produce short utterances. But how many speech pathologists mix-and-match articulation and phonological approaches? How many of us have a solid understanding of when a child is unintelligible due to difficulty being consistent versus not being able to follow a rule, versus not being able to say a sound?
What we need is a better way to help a child by knowing HOW they are being unintelligible, and what we should do about it in speech therapy.
Here is a bit of research on three groups who have worked to better define speech sound disorders. Then we spend the rest of the article creating a one-stop-shop for everything we need to know about types of speech sound disorders so that we can treat, diagnose, and share information quickly and easily.
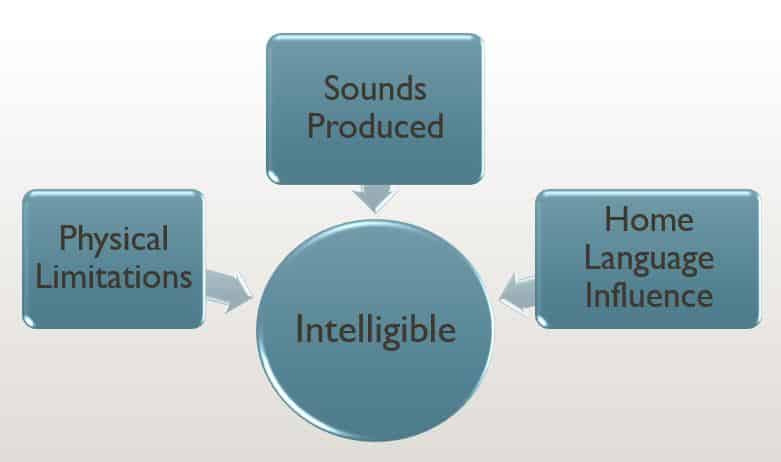
Defining Intelligibility
At its foundation, low intelligibility is the result of a small number of reasons. In each case that we can’t understand a child to some degree, it is due to:
- A physical limitation – E.g., a cleft palate, hearing
- Sounds that can’t be produced because of placement – E.g., articulation
- Sounds that are not produced at the right time because a rule is being broken – E.g., phonology
- A primary language is influencing the sounds a child is trying to produce – E.g., home language influence
It goes without saying that children who fall into the different groups above probably need different interventions to become more intelligible. And if we could decide on better descriptiveness as a field, then we could could align goals, therapy, and research to get faster results.
Subgrouping children into clinically validated subtypes of SSD allows for more precision in the diagnosis, treatment, and prognosis of these disorders. However, to date, there is no single classification system of SSD that is employed uniformly by SLPs (speech-language pathologists).
Lewis, et al 2012 Subtyping Children With Speech Sound Disorders by Endophenotypes
The 3 Prevailing Speech Sound Disorders Research Models
3 Prevailing Speech Sound Disorders Research Models for Defining Intelligibility
There are broadly three primary ways speech sound disorders research has tried to better define low intelligibility. They are grouped based on the cause of the disorder, they are described based on how they are affecting educational outcomes like reading, and they are divided into subclasses based on the type of error that is produced. Let’s review each here and link out to the authors and researchers.
Seven Subtypes of SSD
Lawrence Shriberg has done an insane amount of research on sound disorders. If you are not familiar with his name, know that a lot of his work has influenced what we all covered in grad school. I included six of his studies in the references in the end. I will do my best to sum up some of his ideas on subtyping SSD (Dr. Shriberg, if you are reading this, my apologies in advance!).
Speech sound disorders can be described based on their cause. These are described as the following classes:
- Genetic
- Otitis Media
- Apraxia
- Dysarthria
- Psychosocial Involvement
- 2 groups based on errors
This type of research makes you feel good because we all love to know the cause of an issue. The difficulty that I have as a therapist is that the intake information that I have does not always provide enough information as to the cause, the family might not know the cause, and there aren’t interventions aligned with all of the causes. What do I do in the case of a genetic mutation? Do I intervene differently with Apraxia versus Dysarthria? Shriberg does talk about two groups based on errors, which falls under articulation and phonology, so that helps.
Overall, while cause or etiology might be the most accurate way to describe a speech sound disorder, it doesn’t provide me with the clearest path forward with intervention.
Psycholinguistic Model
Who doesn’t like a big juicy word like “psycholinguistic?” Stackhouse and Wells' 1997 book Children's Speech and Literacy Difficulties: Identification and Intervention: Book II is a cornerstone for speech programs in most English-speaking countries. They tie speech problems to academic problems and show the direct correlation between literacy rates of children who have trouble producing sounds and their intelligibility.
Now we are getting somewhere. This is easy to understand and I see how my role ties to the curriculum and education system. I am a firm believer in tackling literacy and communication together and included many of these ideas in Literacy-Based Intervention.
However, if I am allowed an opinion, it’s this: Our time in clinics is almost devoid of information on school progress. Our time in the schools is so limited that it is very difficult to tackle academic and speech goals simultaneously. While we can incorporate literacy into our therapy (and should!), it’s hard to monitor the child’s literacy rates at the same time we are monitoring intelligibility.
So while I can’t disagree with anything they say, and while I thank them for what they have contributed to the field, I was still left wanting more for my students and clients that really struggle with intelligibility.
Behavioral Appraisal of Speech Sound Disorders
In 2005, Barbara Dodd published work on how to 1) differentially diagnose and 2) treat speech sound disorders. I don’t want the importance of their goal to be lost so let’s break it down. Right out of the gate they are looking for what separates one issue from another, and then try to figure out what to do about it.
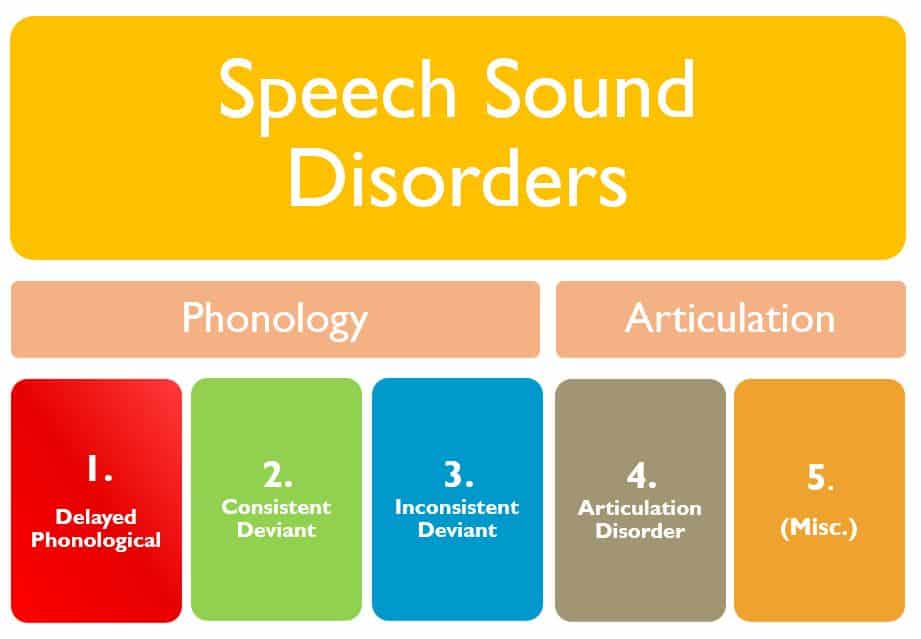
This speech sound disorders research is laid out like our extensive knowledge about language disorders. We have very specific “behaviors” or ways sounds are being said in error, and therefore we should have very specific ways to treat them. The research suggests that phonology should be better described into three groups:
Delayed Phonological: Phonological system similar to younger, typically developing children.
Consistent Deviant Phonological Disorder: Errors that are consistent patterns, but SHOULD NOT be seen by any child at any age. E.g, deleting all syllable-initial consonants.
Inconsistent Deviant Phonological Disorder: Variable productions of the same words or phonological features in the same contexts and across contexts.
This was new information for me when I first read it. I was familiar with delayed phonology of course but had not thought about phonology that should not exist (consistent deviant) or phonology that broke the consistent rule patterns (inconsistent deviant).
These following two groups were more familiar to me and more obviously needed different treatment approaches.
Articulation: An inability to produce a perceptually acceptable version of particular phonemes, either in isolation or in any phonetic context.
Miscellaneous: Low intelligibility attributed to physiological factors such as hearing impairment or craneo-facial anomalies.
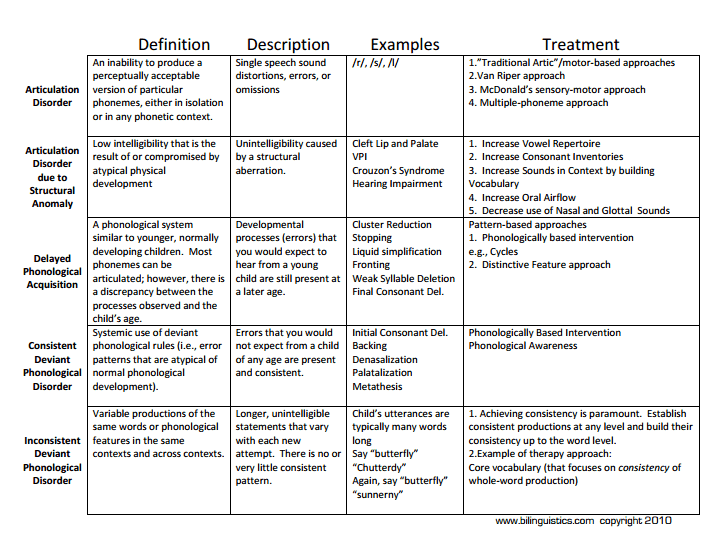
We created two charts to help identify what you should be focusing on, which you can find here: Correctly Matching Speech Sound Disorders to Appropriate Therapy. Use the tree to describe how the child is struggling with intelligibility. Then use the speech sound disorder examples chart to find the therapy types that are most successful. If you want to see how to do this with video examples, check out: Success with Speech Sound Disorders

What is a Speech Sound Disorder?
With that framework in place, we wanted to gather all the information we have on SSDs so that we could easily refer back to it and share with parents and teachers. The ASHA speech sound disorders area is pretty good but it doesn't go into definitions or have the ICD-10 code for speech sound disorder that those of us in the clinic are needing all the time. Plus, "speech sound disorders" can sound scary to parents and not make a lot of sense to teachers. So let's end with some quick definitions, explanations, diagnostic codes, and examples.
Definition and Diagnosis
A speech sound disorder is when an individual has difficulty with the perception, motor-production, or phonological organization of speech sounds. The American Speech‑Language‑Hearing Association (ASHA) practice portal defines SSDs as encompassing both articulation disorders (errors producing individual phonemes) and phonological disorders (systematic error patterns).
Quick Example Table of Errors and Severity
| Error type | Example | Impact on intelligibility |
|---|---|---|
| Articulation (single phoneme) | /r/ → [w] (“rabbit” → “wabbit”) | Mild to moderate |
| Phonological process | Final consonant deletion (“dog” → “do”) | Moderate to significant |
| CAS or motor-planning issue | Inconsistent errors, groping | Severe |
Types & Classification of SSDs
Articulation vs. Phonological
In short: articulation disorders = difficulty physically producing sounds; phonological disorders = difficulty organizing sound patterns and rules.
Other SSD sub-types to know
- Childhood apraxia of speech (CAS) – motor planning/programming issue
- Dysarthria – neuromuscular control issue
- SSD secondary to structural anomalies (cleft palate, hearing loss, syndromes)
ICD-10 coding in U.S. practice
ICD-10 code for SSD in children: F80.0 (Articulation disorder of childhood) or F80.1 (Phonological disorder of childhood) depending on classification — always check latest updates.
Assessment Essentials for SLPs
Standardized tests + non-standardized sampling: Include norm-referenced articulation/phonology tests, spontaneous speech sample, language sampling.
Error pattern analysis: Look for patterns such as fronting, gliding, cluster reduction, stopping — these help identify phonological disorder.
Phonological awareness & literacy link: Research shows children with SSD are at risk for literacy difficulties if phonological awareness is weak.
Key assessment components
| Component | Why it matters | Example item |
|---|---|---|
| Audiology | Rule out hearing cause | PTA pass/fail |
| Oral-motor exam | Identify structural/motor issues | Tongue tie, palate shape |
| Phonemic inventory | Establish baseline | Which consonants correct? |
| Phonological processes | Identify patterns | Final consonant deletion % |
| Phonological awareness | Predict literacy outcomes | Segmentation, rhyming tasks |
Evidence-Based Interventions for Speech Sound Disorders in Children
If you only implement one thing from this section — let it be intensity and frequency.
Fundamentals of treatment
- Improve intelligibility (functional goal)
- Increase phonetic/phonemic repertoires
- Support generalisation to spontaneous speech
Intervention approaches
Here are some evidence-based methods:
- “Integrated Phonological Awareness” – combining phoneme awareness with sound production.
- “Metaphon therapy” – teaching sound contrasts conceptually (e.g., voiced vs voiceless).
- Articulation-based motor training – especially for articulation disorder.
- Intervention intensity matters – more frequent sessions show stronger gains.
Creating a therapy plan (for kiddos)
- Choose target sounds or processes (based on error analysis)
- Plan-for stimulability and functional contexts
- Use a mix of drills + play/naturalistic tasks
- Monitor progress with %-Correct Consonants/Processes
Sample Target Planning
| Target | Rationale | Activities |
|---|---|---|
| /s, z/ sounds | High use in intelligibility, common error | “Snake” game, minimal pair contrast “sip vs ship” |
| Final consonant deletion | Process persists beyond developmental norms | Matching pictures “cat vs ca”, story retell with target words |
| /r/ cluster | Complex production, highly salient | Tongue placement mirror, “pre-school” collage activity |
FAQs (Common Questions asked by parents and teachers)
Can children “grow out” of a speech sound disorder?
Are non-speech oral motor exercises (NSOMEs) useful?
What is the typical age of referral for SSDs?
How often should therapy sessions occur when intelligibility is low?
References:
- Alhaidary, Abdullah. “Treatment of Speech Sound Disorders in Children.” PMC National Center for Biotechnology Information, 2019.
- American Speech-Language-Hearing Association. “Speech Sound Disorders: Articulation and Phonology.” ASHA Practice Portal.
- Dodd B. Differential diagnosis and treatment of children with speech disorder. 2nd. Philadelphia: Whurr; 2005.
- McFaul, Hannah et al. “Applying Evidence to Practice by Increasing Intensity of Speech Sound Disorder Intervention.” BMJ Open Quality, vol. 11, no. 2, 2022.
- Shriberg LD, Kwiatkowski J. Phonological disorders III: A procedure for assessing severity of involvement. Journal of Speech and Hearing Disorders. 1982;47:256–270. [PubMed] [Google Scholar]
- Shriberg LD, Kwiatkowski J. A follow-up study of children with phonologic disorders of unknown origin. Journal of Speech and Hearing Disorders. 1988;53:144–155. [PubMed] [Google Scholar]
- Shriberg LD, Kwiatkowski J. Developmental phonological disorders I: A clinical profile. Journal of Speech and Hearing Research. 1994;37:1100–1126. [PubMed] [Google Scholar]
- Shriberg LD, Kwiatkowski J, Best S, Hengst J, Terselic-Weber B. Characteristics of children with phonologic disorders of unknown origin. Journal of Speech and Hearing Disorders. 1986;51:140–161. [PubMed] [Google Scholar]
- Shriberg LD, Lewis BA, Tomblin JB, McSweeny JL, Karlsson HB, Scheer AR. Toward diagnostic and phenotype markers for genetically transmitted speech delay. Journal of Speech, Language, and Hearing Research. 2005;48:834–852. [PubMed] [Google Scholar]
- Shriberg LD, Tomblin JB, McSweeny JL. Prevalence of speech delay in 6-year-old children and comorbidity with language impairment. Journal of Speech Language and Hearing Research. 1999;42:1461–1481. [PubMed] [Google Scholar]
- Stackhouse J, Wells B. Children's speech and literacy difficulties. London: Whurr; 1997.










Whatever happened to phonological processes analysis.?
Yes! What I think this research does better than what we have in the past is that it dives one level deeper than phonological process analysis. Dodd’s work actually better defines it as three separate groups. So not only do you get an idea of the processes that are being used or creating errors, but specific ways to treat them. Check out the CEU course above because it’s 90 minutes of discussing this very topic.
I updated the links to this blog post and added more resources due to so many of your responses. Thank you for the suggestions.
On your chart, where would CAS fall?
CAS is actually not part of this chart because in the research it is considered separately because of its uniqueness like fluency and hearing loss influenced speech issues. Highly unintelligible, inconsistent phonology issues are often confused with CAS. However with CAS the syllable sizes are tiny while phonology is highly unintelligible but utterance length is not affected. Here is some Apraxia-specific information: (Childhood) Apraxia Causes, Characteristics, and Resources 5 Tips for Working with Childhood Apraxia of Speech